Tendosynovitis
Here we explain the onset, the causes, the symptoms and possible treatments of tendosynovitis.
What is Tendosynovitis?
Tendons are composed of connective tissue and attach muscles to bones. They are surrounded by so-called tendon sheaths which help to protect the most strained parts. These sheaths are composed of two different types of layers which are filled with synovial fluid to keep the tendon lubricated and at the same time minimize pressure and friction. But repeated stress may cause inflammation between the layers – which is called 'tendosynovitis' (tendovaginitis).
Chronic muscle tension over an extended period of time may lead to tendosynovitis. This can cause swelling of the tendon and the tendon sheath. Stretching or moving the tendon is now painful.
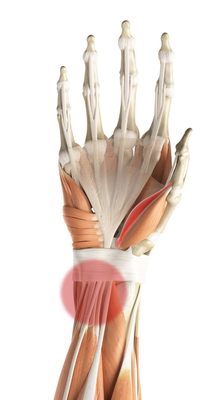
The most common site for tendosynovitis is the wrist. Depending on the tendons affected, a carpal tunnel syndrome or trigger finger may occur. Tendon sheath inflammations are less common in the arms or feet.

Causes
The inflammation of the tendon sheath occurs between the two layers of the sheath surrounding the tendon. The main reasons for this are repetitive, unilateral movements or a poor posture. Tenosynovitis rarely occurs in the course of rheumatic diseases.
Office workers are particularly likely to be affected. Furthermore, musicians, mechanics and athletes are also at risk. In general, the inflammation is a repair process responding to muscle tension.
Symptoms
In most cases, the pain accompanying the tendosynovitis occurs when performing the wrong or unilateral movement that lead to the inflammation. In many cases, it is possible to identify the affected area thanks to the swelling of the tendon or tendon sheath and sometimes even nodules. Furthermore, the inflamed area is sensitive to pressure. Once the disease reaches an advanced stage, the patient feels the stabbing pain even at rest.
Sometimes adhesions form between the tendon and the surrounding tendon sheath inhibiting the tendon gliding. In this case, patients report a noticeable friction and clearly audible crackling sound. The significant restriction of mobility is the result of this inflammation.
Diagnosis
Tenosynovitis is diagnosed based on a simple physical exam and the patient's medical record. Imaging techniques such as x-ray or the like are usually not necessary. A blood test can help rule out rheumatic diseases as the cause of the inflammation. The inflammation heals within a few weeks of resting and immobilizing the affected area.
Prevention
In order to prevent a tendon sheath inflammation, it is important to reduce specific unilateral movements and avoid overloading the tendon. This means, for example, taking regular breaks at work and adopting a correct ergonomic posture of the legs and the arms when sitting.
Make sure to warm up the muscles if the inflammation occurred during sports and to minimise the risk of overuse and general injuries. Stretching regularly is also highly recommended. Furthermore, using the proper technique and wearing the right equipment helps to prevent incorrect loading.
Non-surgical treatment
After receiving the diagnosis of tenosynovitis, it is important to avoid painful movements. In the first three to five days, cool packs can be used to treat the inflammation. Anti-inflammatory drugs or cortisone injections are additional treatment options.Orthopedic supports and ortheses. help to immobilise and relieve the affected body part.
Ultrasound, cross friction, osteopressure, taping or impuls vacuum massages may help to reduce the muscle tension and to promote the healing process. Specific physiotherapy starts with stretching exercises, which are gradually supplemented during the regeneration phase by exercises to build muscle.
Operation and aftercare
Surgery may be an option if the symptoms still have not improved after three to six months. This can be performed as an outpatient procedure. The surgeon removes the constricting, inflamed or swollen tissue. The objective is to give the tendon more room to move – without the painful friction. Only a small incision is required.
The tendon should be moved slowly again immediately after the operation, but without putting strain on the scar or pulling the wound, thereby ensuring that no surrounding nerve grows together incorrectly with the scar tissue. Usually, the stitches may be removed after ten days. As with any operative procedure, complications may occur. During the surgery, a nerve may be injured which can lead to sensory disturbances or movement restrictions. However, the risk is relatively small. After two to four weeks the affected body part can be moved free of pain. And after two months the affected area reaches its full load-bearing capacity.






