Rhizarthrosis
This article will explain the development, causes, symptoms, and treatment options for rhizarthrosis.
What is Rhizarthrosis?
Rhizarthrosis relates to Arthrosis, which is the abrasion of the thumb saddle joint. It is the most common type of degenerative joint disease found in this area of the hand. Rhizarthrosis can cause pain, reduced strength when gripping (with the effected hand) and limited mobility. These symptoms are caused by chronic wear of cartilage, which causes the articular surfaces to rub against each other. If left untreated, it can lead to progressive loss of cartilage in the thumb saddle joint. Common causes are incorrect or too much strain. The good news is that there are many conservative and surgical treatment options.

Causes
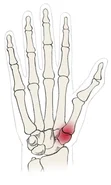
Within the thumb saddle joint, the first metacarpal bone sits on the large trapezium bone of the wrist like a ‘saddle’. To give the thumb its flexibility, the saddle joint only has a weak bone anchoring. It receives its stability from muscles and ligaments. The thumb saddle joint is relatively small but also one of the most strained joints of the body as it enables the gripping and holding function of the hand.
The main causes of rhizarthrosis are permanent overloading as well as misalignment of the joint position. If the ligaments and muscles are weakened, the thumb saddle joint can become unstable, leading to improper strain.
As is common with degenerative diseases, the risk of rhizarthrosis increases with age. One in four women and one in twelve men over 70 are estimated to be affected, however, even younger people can suffer from it. The disease increasingly occurs within families and in post-menopausal women. This suggests that genetic predispositions, as well as hormonal causes, play a role.
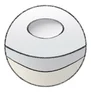
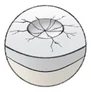
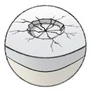
Causes and consequences of Arthrosis
Symptoms
The loss of cartilage caused by overloading and misalignment of the joint causes joint pain for those affected. Attempting to stabilise the joint through muscles results in an uneven load, which leads to muscle pain. Over time, this can lead to muscle shortening and changes in the joint capsule, which will effectively cause limited mobility.
The symptoms will be particularly apparent during holding and turning movements, such as when turning a key or opening a screw cap.
Diagnosis
The diagnosis of rhizarthrosis is made by a doctor through close examination and palpation of the thumb saddle joint. This is then confirmed using an X-ray.
Prevention
As a rule, rhizarthrosis is initially treated conservatively. Surgery is usually unnecessary in the early stages. To avoid a progression of cartilage loss, prevention and therapy for the condition largely mean the same thing. Prevention is key when it comes to this condition.
It is important that the joint elements are positioned as optimally to one another as possible, particularly while straining the joint. That way, the pressure in the joint is evenly distributed. Misplacements in the joint position have to be balanced out as soon as possible. Excessive and improper strain in everyday life should be avoided.
Non-surgical treatment
Treatments for rhizarthrosis are based around the extent of the joint’s abrasion and the intensity of the pain experienced as a result of the condition.
To take the strain off the diseased joint and to stabilise it, you can use special thumb splints (orthoses). Lighter models specifically stabilise the thumb saddle joint under strain without restricting the mobility of the hand. If the rhizarthrosis is in a more advanced stage, an orthosis is recommended as this provides more stability to the saddle joint and prevents hyperextension in the joint at the base of the thumb.
Acute pain can be relieved through cooling with ice, the use of anti-inflammatory painkillers, and through the application of ointments.
Further treatment options are cortisone injections, hand, ergo- and physiotherapy as well as acupuncture, among others.
Operation and aftercare
If all conservative treatment options are unsuccessful or if the rhizarthrosis is already at an advanced stage, there are surgical alternatives. Treating rhizarthrosis surgically is a rescue operation and is only opted for when all other measures have been exhausted. Doctors decide individually on a case-by-case basis which procedure is most suitable.
A common procedure is the removal of the trapezium bone. To do this, the first metacarpal bone is fixed with a tendon so that it doesn’t slip into the resulting hole. After the operation, the thumb is initially immobilised for six weeks, however, it can take up to twelve weeks for a full recovery. As one of the joint elements is now missing, stabilising the saddle joint when exposed to strain is also recommended
Naturally, other surgical procedures can be employed, such as immobilisation of the thumb saddle joint (arthrodesis) or the insertion of an artificial joint.




